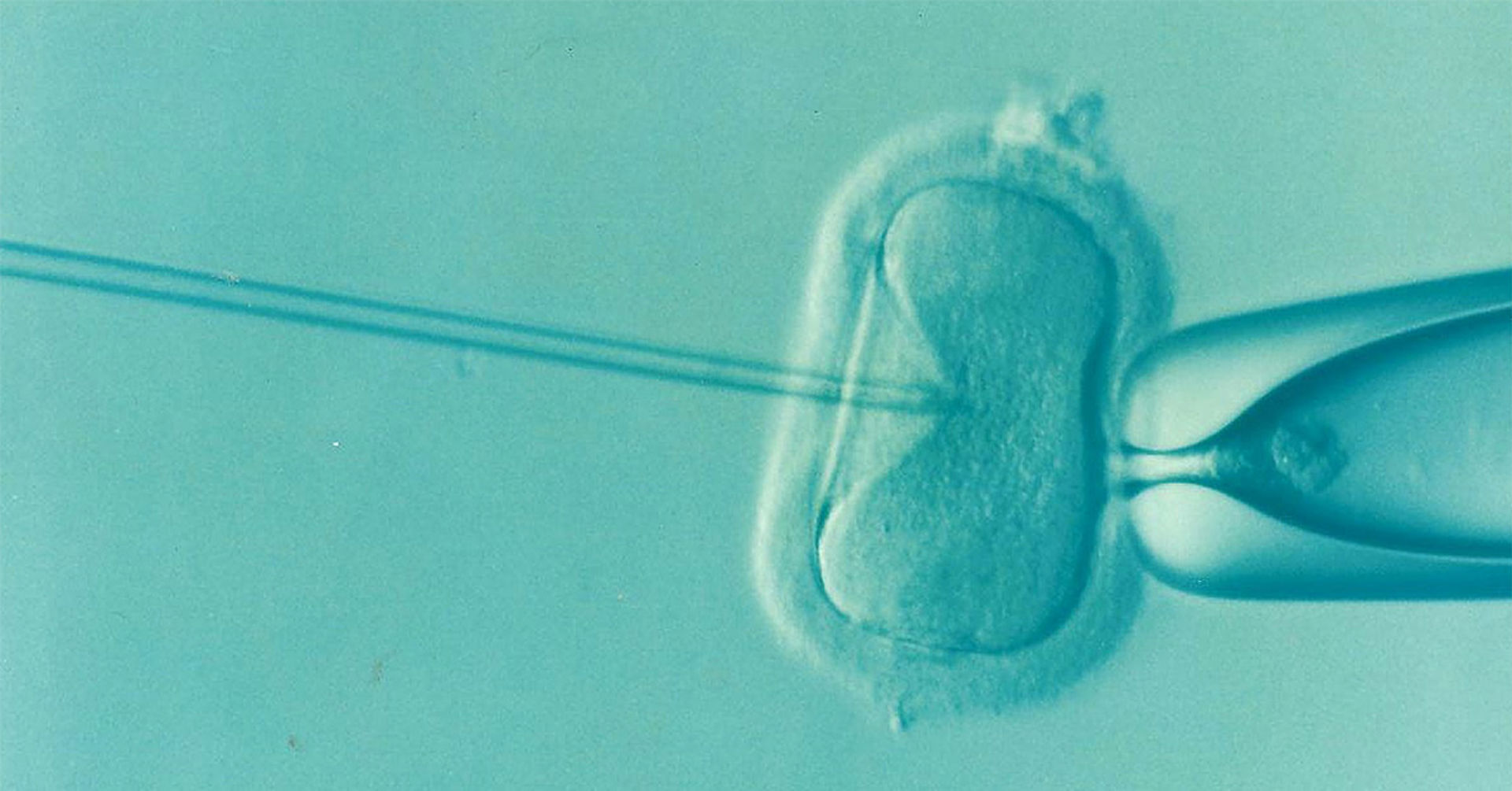
In-vitro-fertilization (IVF), a fertility treatment that involves fertilizing eggs in the laboratory and later implanting them in the uterus, has been a source of hope for many people struggling to conceive. However, the multi-step process is complex, and the overall live birth rate after IVF treatment is only 20-40% in females younger than 40 in the United States. One of the reasons for this low success rate is that it’s very difficult for doctors to determine which lab-grown embryos are most likely to result in a successful pregnancy, so many people seeking IVF must go through multiple rounds of treatment.
Now, scientists at University of California San Diego School of Medicine have uncovered a noninvasive approach that can be used to better predict the quality of lab-grown embryos. The new method works by detecting small particles of genetic material, called exRNAs, that are left behind in the liquid media young embryos are grown in. The findings were published January 10, 2024 in Cell Genomics.
"Unfortunately, IVF success still involves a big element of chance, but that’s something we’re hoping our research can change," said co-senior author H. Irene Su, MD, professor in the Department of Obstetrics, Gynecology and Reproductive Sciences at UC San Diego School of Medicine and a reproductive endocrinologist at UC San Diego Health. "Right now, the best way we have to predict embryo outcome involves looking at embryos and measuring morphological characteristics or taking some cells from the embryo to look at genetic makeup, both of which have limitations."
Instead of relying on either visual characteristics or biopsies of embryos, the new approach works more like a blood test by detecting molecules in a sample of fluid. However, instead of that sample coming from the embryos themselves, the researchers are able to analyze embryos by studying the leftover medium used to grow them. This means that the new approach is completely noninvasive and involves no extra steps on the part of the patient.
"IVF is challenging enough as it is, so it was extremely important to us that our research didn’t interfere with this already-delicate process," said Su. "What we’ve done is more akin to looking at what’s left behind at an archeological site to help us learn more about who lived there and what they did."
While DNA contains all the instructions our cells need to develop and function, they also need RNA, another type of genetic material, to help carry out these instructions. Most RNA is found inside of cells, but some RNA molecules, called exRNAs, are released by the cell into their surroundings while the cell completes its various functions.
Scientists are still unsure of the precise biological function of exRNAs, but their discovery in the early 2000s has opened up new avenues in biomedical research and medicine, offering insights into cell-to-cell communication and disease processes, as well as potential diagnostic and therapeutic applications.
"It’s really only in the last decade that we have started to uncover the uses for exRNAs, and there could be countless other applications we haven’t yet discovered," said co-senior author Sheng Zhong, PhD, professor in the Shu Chien-Gene Lay Department of Bioengineering at UC San Diego. "This is just the beginning."
By analyzing the exRNA in culture media for embryos at five different developmental stages, the researchers identified about 4,000 different exRNA molecules per stage. These exRNAs correspond to the many different genes that are expressed in embryos at each developmental stage.
"We were surprised by how many exRNAs were produced so early in embryonic development, and how much of that activity we could detect using such a minute sample," said Zhong. "This is an approach where we can analyze a sample from outside a cell and gain an incredible amount of insight into what’s happening inside it."
The researchers used the data to train a machine learning model to predict the embryo’s morphology based on the exRNAs it produced. They found that their model was able to replicate the morphological measurements used in current embryo tests, suggesting exRNAs were a promising predictor of embryo quality.
Still, the researchers caution that it will take additional research to confirm whether their test can be used directly to predict positive IVF outcomes, such as successful births.
"We have data connecting healthy morphology to positive IVF outcomes, and now we’ve seen that exRNAs can be used to predict good morphology, but we still need to draw that final line before our test will be ready for primetime," said Su. "Once that work is done, we hope this will make the overall process of IVF simpler, more efficient, and ultimately less of an ordeal for the families seeking this treatment."
Co-authors of the study include: Qiuyang Wu and Zhangming Yan at UC San Diego, Zixu Zhou at Genomo Inc. and Megan Connel, Gabriel Garzo, Analisa Yeo and Wei Zhang at Reproductive Partners San Diego.
This study was funded, in part, by the National Institutes of Health (grants R01HD107206, R01GM138852 and DP1DK126138) and a Kruger research grant.
Disclosures: Sheng Zhong is a founder and board member of Genemo, Inc.